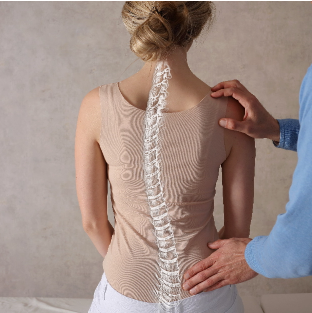
Spinal deformities are defined as an abnormality in the alignment of the spine.
They can cause many problems in the body, including pain, neurological dysfunction, and issues pertaining to mobility. There are some spinal deformities that involve multiple vertebrae and cause pain, numbness, and instability in the back. A surgical procedure that can capture the repair of 6 or more vertebral bones in reconstructive surgery is known as a complex spinal surgery.


Some spinal deformities may be corrected with the use of a brace or other exterior apparatus, medications, and certain physical therapy treatments can also correct some spinal deformities. The types of treatment options that are recommended for spinal deformities align with a patient’s age, overall health, and the presence of associated symptoms.
Surgical procedures can become life-changing events for patients living with spinal deformities. For some patients with deformities like kyphosis, scoliosis, or spondylolisthesis, a spinal deformity surgery can transform their lives – from improving their day-to-day activities to achieving things they never before thought possible
Dr. Jeremy Smith, M.D., has specialized expertise in spinal deformity surgery. He has been highly sought after in the field for years, by both patients and fellow surgeons alike.
Although not all spinal deformities require surgery, the most extreme conditions are much improved by it. Some examples of such conditions are scoliosis, kyphosis, lordosis, spondylolisthesis, spinal tumors, spinal fractures, and neuromuscular deformities.



Scoliosis is a type of spinal deformity where an abnormal curve in the spine has developed. There are different types of scoliosis: idiopathic (no certain cause of the disease), congenital (an abnormal curve that you’re born with), and neuromuscular (associated with nerve disorders).
Several factors contribute to whether your surgeon recommends how to treat your scoliosis. The severity of the condition, health, age, and other symptoms play a role in whether surgery is the right treatment to correct your spinal deformity. Patients may experience severe curvature, progression, pain, and even respiratory issues associated with scoliosis.
SURGICAL TECHNIQUES
There are a number of surgical treatments available when addressing spinal deformities, including spinal fusion (when multiple spinal vertebrae are bonded together), instrumentation (attaching rods and screws in order to stabilize the spine), and a number of minimally invasive procedures (such as replacing damaged/diseased vertebral discs with artificial ones).
RISKS
No surgery is without risk. Some risks from surgery for a spinal deformity may include damage to the spinal cord, cardiovascular, and pulmonary complications, infection, or nerve root injury. However, there are times when the best possible outcome for a spinal deformity comes from a surgical option. Many of these risks have a very low rate of occurrence during surgery.
ADULTS VS. PEDIATRIC SCOLIOSIS SURGERY
While it is possible for most children to outgrow their scoliosis by way of the help of a back brace, adult scoliosis surgery may be necessary to perform so that the developing curvature of the spine may be halted as much as possible.
POST-OPERATIVE CARE AND REHABILITATION FOR SCOLIOSIS PATIENTS
The average time it takes to return to normal activities after receiving scoliosis back surgery varies depending on the complexity of each case. For patients with just one spinal curvature, there will likely be one 10-inch scar that is present after surgery.


Kyphosis is the abnormal curvature of the upper back. The 3 types of kyphosis are postural (caused by bad posture), Scheuermann’s (a structural deformity), and congenital (a deformity present since birth).
In severe cases of kyphosis, a patient may experience a curve that affects their ability to breathe or look straight, neurological compromise, and/or pain – surgery may become imperative in order to properly treat the condition in the most effective way. These extreme symptoms may be caused by structural issues, spinal fractures, or osteoporosis.
Kyphosis may also be improved with physical therapy, bracing, and/or exercise. Some additional surgical options for treating kyphosis include an osteotomy, spinal fusion, and vertebral column resection. Imaging and other robust testing will inform your surgeon as to which surgical or non-surgical option is the best treatment for you.
Surgery performed to address Kyphosis can sometimes cause complications (such as infections). Your surgeon and medical team will prepare you by giving you the best practices for managing your post-operative self-care.
Surgery performed to address Kyphosis has a highly proven success rate in the US, with the majority of adults regaining proper posture and other desired surgical outcomes.
Corrective surgery for kyphosis can usually be performed within 4-5 hours. After surgery, patients usually recover in the hospital over 3-4 days and at-home recovery usually occurs over 4 to 6 weeks. Your surgeon will prescribe pain medications and physical therapy treatments to help you regain your strength and mobility.

There are many different types of lordosis. Cervical lordosis surgery addresses the abnormal curve of the spine in the neck region, caused by pushing the neck forward. Posterior lordosis is caused by uneven posture or injury. Congenital lordosis is caused by genetics. Neuromuscular lordosis is caused by the presence of another condition, such as muscular dystrophy, cerebral palsy, or spina bifida.
During a reverse cervical lordosis surgery, a surgeon realigns the spine and restores loss. Lumbar lordosis corrective surgery uses a surgical approach to fuse the vertebrae together in order to restore the region.
Patients suffering from extreme curvature or neurological deficits are prime candidates for lordosis surgery. An osteotomy (surgical cutting/removing of the bone), vertebral column resection (surgical removal of vertebrae), and spinal fusion (when multiple vertebrae are bonded together) are different approaches to lordosis surgery. The goal of lordosis surgery is to straighten and correct the alignment of the spine. Dr. Smith specializes in minimally invasive surgeries for lordosis.
The recovery from a lordosis surgery can last 1-4 days post-op in the hospital and extend to several weeks of at-home recovery. The recovery time for a minimally invasive surgery measures success in far less time. Your doctor will prescribe you pain management medications as well as physical therapy treatments once you have passed your initial recovery.
Spondylolisthesis is a spinal disorder. It occurs when a vertebral bone slips forward compared to the bone below it. Degenerative spondylolisthesis occurs due to arthritis, while isthmic spondylolisthesis occurs as the result of a fracture. The most common area for spondylolisthesis to occur is within the bottom of the lumbar spine between L4-L5 and L5-S1.
Your doctor may prescribe rest, physical therapy, and anti-inflammatory medications to treat your spondylolisthesis, as non-surgical options. However, symptoms such as nerve compression, spinal instability, or progressive slippage may require surgical correction to relieve and stabilize the spine.
Your doctor may want to treat your spondylolisthesis with any number of surgical options, including a spinal fusion. Minimally invasive procedures take place over a couple of hours and can be outpatient surgeries. These minimally invasive procedures allow patients to experience a faster recovery time and pose less risk to the patient.
Patients can expect to experience shorter recovery times with minimally invasive surgeries – however, most patients will experience a full recovery between 18-24 months, as the nerves take up to 2 years to heal. Minimally invasive surgeries create smaller scars because the incisions are much smaller than traditional surgery.
Dr. Jeremy Smith, M.D., has a very high rate of success with minimally invasive procedures and has been performing them on patients for many years. After your spondylolisthesis spinal surgery, you can expect to return to normal daily activities within a few weeks.

There are a few types of tumors that can occur in the spine:
Benign tumors: non-cancerous tumors
Malignant tumors: diseased and infectious tumors that may spread to other areas of the body if not removed quickly
Metastatic tumors: a tumor that has spread from a primary site to the spine (or other secondary location).
Cancerous tumors can spread very rapidly and it is important to begin treating them right away. An early diagnosis of these tumors leads to the best possible patient outcome. Magnetic resonance imaging (MRI), myelography, post-myelo-computed tomography, and bone scan are the mainstay of evaluation of tumors of the spine.
SURGICAL APPROACHES
Spinal tumors can be treated in a variety of ways, but surgery is one of the most common treatments. Tumor resection is a surgery where laminae are removed from the spine to access the spine canal and remove the tumor. Decompression surgery relieves pressure on the spinal cord and nerve roots by removing part or all of the tumor from the spine. During these surgeries, your surgeon will also stabilize your spine to help with structural support.
While there is risk associated with the surgery, a minimally invasive approach lowers the risks of infection and complications. This surgery may take place over a couple of hours. Some side effects from this surgery can include postoperative pain and reduced range of motion. Initial recovery from this type of spinal surgery is usually 6-12 weeks.
Dr. Smith successfully performs spinal surgery with the goal of removing spinal tumors on a regular basis. Dr. Smith works very closely with specialized oncologists in order to give his patients the highest value of care.
Spinal fractures are actually far more common than one may think. They can occur due to trauma, osteoporosis, and pathological conditions. Classifying spinal fractures fall into two categories: stable (the bones have not moved out of place) or unstable (the bones have moved out of alignment). Depending on your fracture, it may not require surgery to heal.
Minimally invasive surgeries can be applied to several spine fracture conditions, including vertebral augmentation, spinal fusion, and instrumentation. Recovering from spinal surgery from a fracture usually takes 2-6 weeks. It is not recommended that patients drive before that time frame has ended. Staying in shape, staying active and adhering to precautions are the best way to facilitate healing after surgery. Stretching is also an important part of the healing process.


The spine can also become deformed from neuromuscular conditions, such as muscular dystrophy, cerebral palsy, and spina bifida. Muscular dystrophy weakens and wastes muscles – it is a hereditary disease. Cerebral palsy is caused by brain damage at birth and is a disorder of movement, muscle and posture in the body. Spina Bifida is a birth defect where the spinal cord does not fully develop.
Managing neuromuscular spinal deformities are challenging as they can be debilitating and advance quickly. They also cause a number of other issues as a result of the impact they have on the spine and the body. Surgery through stabilization, spinal fusion, or muscle release, are all options that a patient who suffers from neuromuscular deformities might consider in order to correct their condition.
There are also post-operative care options available as well as multidisciplinary support for patients with neuromuscular deformities.
Can spinal deformity be corrected?
Yes! There are a number of surgical and non-surgical options available for patients with various spinal conditions.
What is the goal of complex spinal deformity surgery?
The goal of complex spinal deformity surgery is to improve posture/alignment, reduce pain, reduce dysfunction and resolve issues with mobility by repairing 6 or more vertebral bones in this reconstructive surgery.
Is spinal deformity surgery high risk?
Every surgical procedure has a set of risks associated with it, however, for patients suffering from severe life-limiting spinal deformities, a spinal deformity surgery can transform their lives for the better.
What are the most common complications?
The most common complication from a spinal deformity surgery is infection - this can be carefully monitored and tended to post-surgery, and therefore, there is high likelihood it can be avoided.
Who is not a good candidate for this type of surgery?
The types of treatment options that are recommended for spinal deformities align with a patient’s age, overall health, and the presence of associated symptoms. These factors may or may not make you eligible for this type of surgery.
How should I prepare for deformity correction and stabilization?
A stabilization procedure may be necessary before any corrective surgery, such as an osteotomy, pedicle subtraction osteotomy, vertebral column resection, or spinopelvic fixation - each of which involve the removal of, or instrumentation into, bone. This will help the region to be better prepared for a spinal deformity surgery. You should also participate in routine exercise and quit smoking before all procedures and surgeries.